Skin is our body’s largest organ and serves as the first line of defense against external threats. However, skin can also be prone to various conditions, some of which are benign yet bothersome. Milia is one such common skin condition that affects people of all ages. In this comprehensive guide, we will delve into what milia is, its causes, types, prevention, and treatment options.
Chapter 1: Understanding Milialar
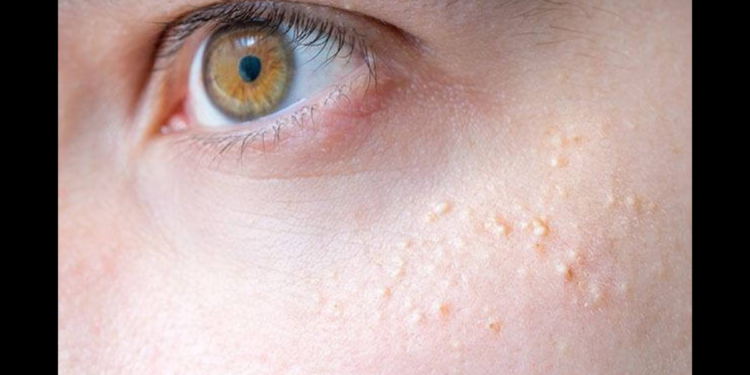
Milialar , pronounced as “mil-ee-uh,” are small, white or yellowish bumps that appear on the skin’s surface. They are often mistaken for whiteheads or pimples, but they are quite different. Milia are cysts filled with keratin, a protein that makes up the outer layer of the skin, hair, and nails. Unlike pimples, milia do not have an opening or pore, making them challenging to extract. They are typically painless and not contagious.
Chapter 2: Types of Milialar
Milialar can be categorized into several types based on their origin and location on the body. Understanding these different types can help in diagnosis and treatment. The common types include:
- Primary Milialar : These are the most common type and occur for no apparent reason. They often appear on the face, particularly around the eyes, nose, and cheeks.
- Secondary Milialar : These Milialar develop as a result of another skin condition, injury, or trauma. Blistering, burns, or skin resurfacing procedures are common triggers.
- Neonatal Milialar : Also known as “baby Milialar ,” these tiny white bumps often appear on newborns’ faces. They typically disappear within a few weeks without any treatment.
- Milia en Plaque: This is a rare form of Milialar that appears in a group or patch on the face or neck. It can be associated with other skin conditions like discoid lupus erythematosus.
Chapter 3: What Causes Milia?
Understanding the underlying causes of Milialar is crucial for prevention and effective treatment. Some common causes include:
- Skin Trauma: Injury or damage to the skin, such as burns, blisters, or excessive sun exposure, can trigger milia.
- Skin Care Products: The use of heavy or occlusive skincare products, especially those containing mineral oil or petrolatum, can clog pores and lead to milia formation.
- Genetics: Some individuals may have a genetic predisposition to developing milia.
- Topical Steroid Use: Long-term use of topical steroids can disrupt the skin’s natural exfoliation process and result in Milialar .
- Underlying Skin Conditions: Certain skin conditions, like epidermolysis bullosa or porphyria cutanea tarda, can increase the risk of milia.
Chapter 4: Prevention of Milialar
Preventing Milialar can be more manageable than treating it once it has formed. Here are some steps you can take to reduce the risk of developing milia:
- Gentle Exfoliation: Regular exfoliation with a mild exfoliant can help remove dead skin cells and prevent the buildup of keratin.
- Choose Non-comedogenic Products: Opt for skincare and makeup products labeled as non-comedogenic, as they are less likely to clog pores.
- Sun Protection: Wear sunscreen daily to protect your skin from sun damage, which can contribute to Milialar formation.
- Avoid Heavy Moisturizers: If you are prone to Milialar , use lightweight moisturizers and avoid heavy creams.
Chapter 5: Treatment Options
While Milialar often resolve on their own over time, some cases may require intervention. Here are common treatment options:
- Extraction: A dermatologist can safely extract Milialar using a sterile needle or scalpel. This procedure should not be attempted at home.
- Chemical Peels: Chemical peels can help exfoliate the skin and reduce the appearance of Milialar .
- Topical Retinoids: Prescription retinoids like tretinoin can promote cell turnover and prevent Milialar .
- Cryotherapy: Liquid nitrogen is used to freeze and remove Milialar .
- Laser Therapy: In some cases, lasers may be used to target and remove Milialar .
Chapter 6: When to See a Dermatologist
If you have persistent Milialar , milia en plaque, or if they are causing cosmetic concerns, it is advisable to consult a dermatologist. They can provide an accurate diagnosis and recommend the most appropriate treatment.
Chapter 7: Conclusion
Milialar may be a common skin condition, but it can be a source of frustration and self-consciousness for those who have it. Understanding what milia is, its causes, and available treatment options can empower individuals to take better care of their skin and seek professional guidance when needed. Remember that skin health is an essential aspect of overall well-being, and with the right knowledge and care, you can keep your skin looking and feeling its best.




More Stories
Is Nahraan Kids Multivitamin the Right Choice for Your Child? A Complete Honest Review of Halal Nutrition Options
The Ultimate Guide to Brazilian Jiu Jitsu in Littleton, CO
Your Complete Guide to Professional Cyst and Lipoma Care in Orange County